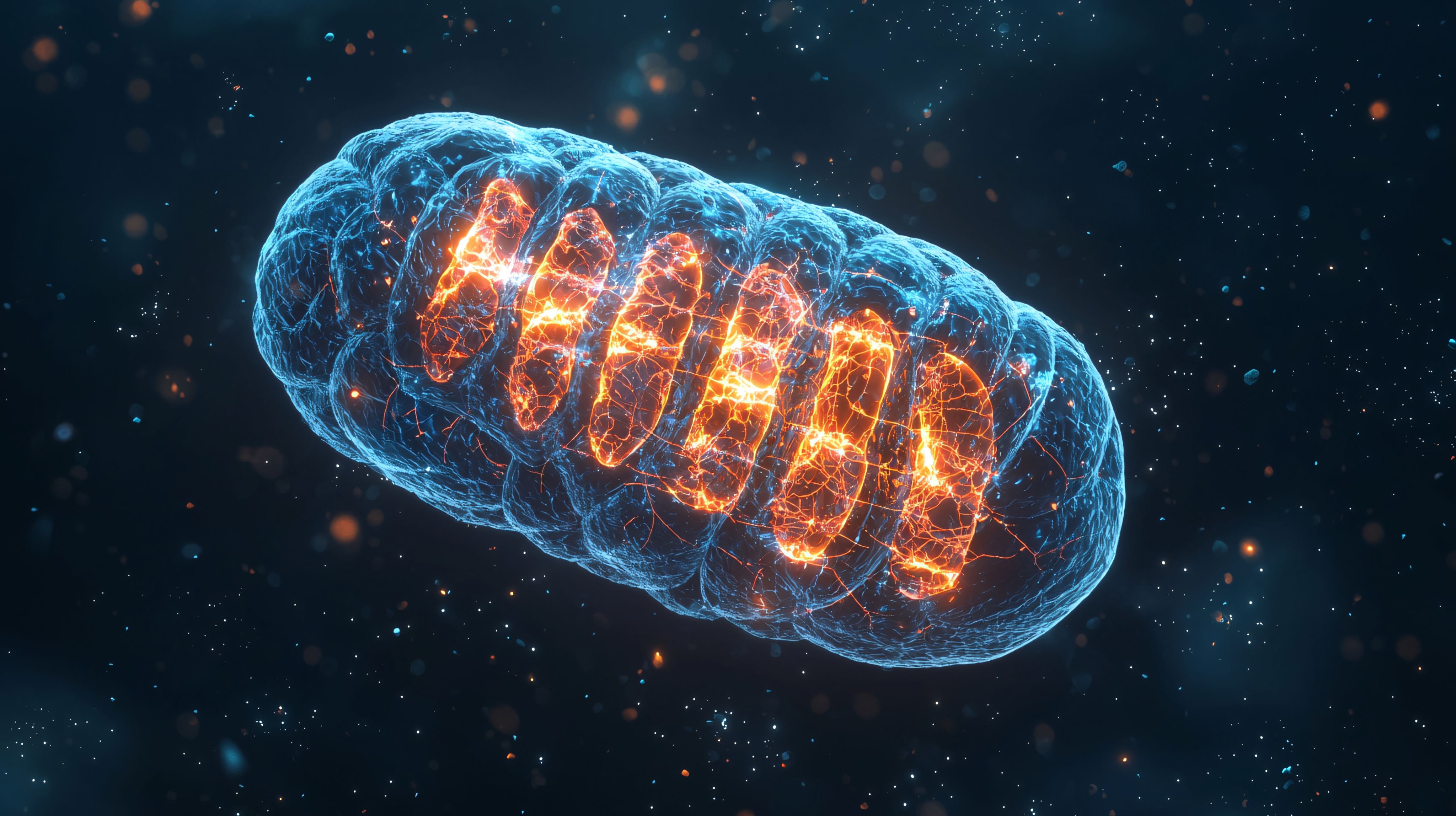
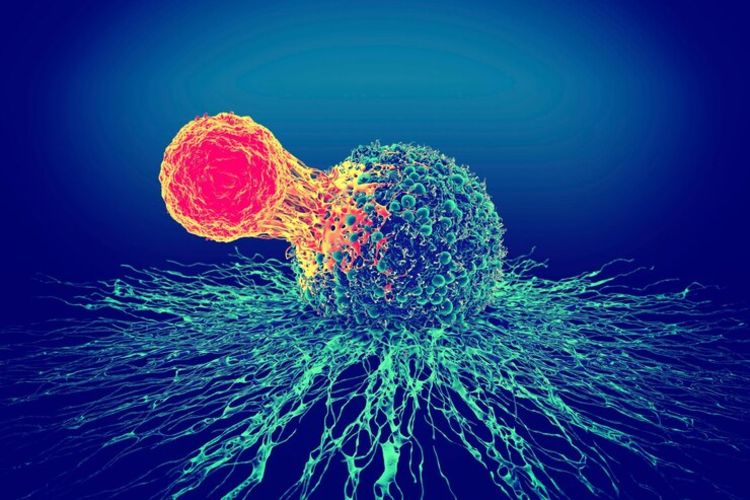
Shock to cancer cells
Electric pulse and calcium can jointly destroy cancer
A study by researchers from the Wroclaw Medical University- Dr. Anna Szewczyk, Dr. Nina Rembiałkowska, Prof. Jolanta Saczko, and Prof. Julita Kulbacka - conducted in collaboration with a team from Vilnius University and the University of Wroclaw, indicates the potential of a therapy that combines short electric pulses with calcium in the fight against resistant colon cancer. The new method kills cancer cells, weakens their "stem cells" and awakens the immune system. This is one promising therapeutic pathway in oncology.
Shock to cancer cells: podcast
Click here to listen!
Live calcium
It has long been known that electricity can do remarkable things to cells - opening their membranes, facilitating drug transport, and even destroying tumors. But scientists from Wroclaw and Vilnius have gone a step further. Their weapon? A nanosecond-long electrical impulse and... a calcium ion.
Calcium electroporation (CaEP) is a method that, in recent years, has been gaining recognition as a stand-alone anti-cancer therapy – especially in countries such as Denmark and Germany.
– I had the opportunity to participate in a procedure using CaEP to treat breast cancer during my internship in Copenhagen in 2016, recalls Dr. Anna Szewczyk, the first author of the study. – This experience reinforced my belief that this method is not only practical but also safe and relatively minimally invasive. I see great potential in combining CaEP with classical therapies, such as chemotherapy or immunotherapy. Such an approach can enhance the therapeutic effect and broaden the spectrum of clinical applications of this method – Dr. Szewczyk emphasizes.
In a study described in the article Calcium electroporation induces stress response through upregulation of HSP27, HSP70, aspartate β-hydroxylase, and CD133 in human colon cancer cells published in the Springer Nature publishing group's journal Biological Research, researchers compared two types of electrical pulses - microsecond (µsEP) and nanosecond (nsEP) – for their effects on colon cancer cells, including those resistant to chemotherapy.
The results are unequivocal: nanosecond pulses combined with calcium (so-called nanosecond calcium electroporation, nsCaEP) cause severe damage to mitochondria, a sharp increase in oxidative stress, loss of energy, and activation of cell death mechanisms

Faster, deeper, more effective
The difference between microsecond pulses on nanosecond pulses? Crucial. While microsecond pulses mainly affect the cell membrane, nanosecond pulses penetrate much deeper - they reach organelles, including mitochondria and the endoplasmic reticulum. This is where the cellular drama occurs - disturbed calcium balance, damaged mitochondria, and an explosion of free radicals.
In the researchers' experiments, the level of reactive oxygen species (ROS) increased fivefold in nsCaEP-treated cancer cells. At the same time, the level of ATP—the cellular energy currency—fell dramatically. Cancer cells, which need a huge amount of energy to grow and divide, couldn't stand it.
Interestingly, healthy cells responded more mildly to the therapy. This suggests that selectivity can be achieved – destroying cancer while sparing healthy tissue.
One weapon, three targets
Therapy based on nsCaEP works threefold:
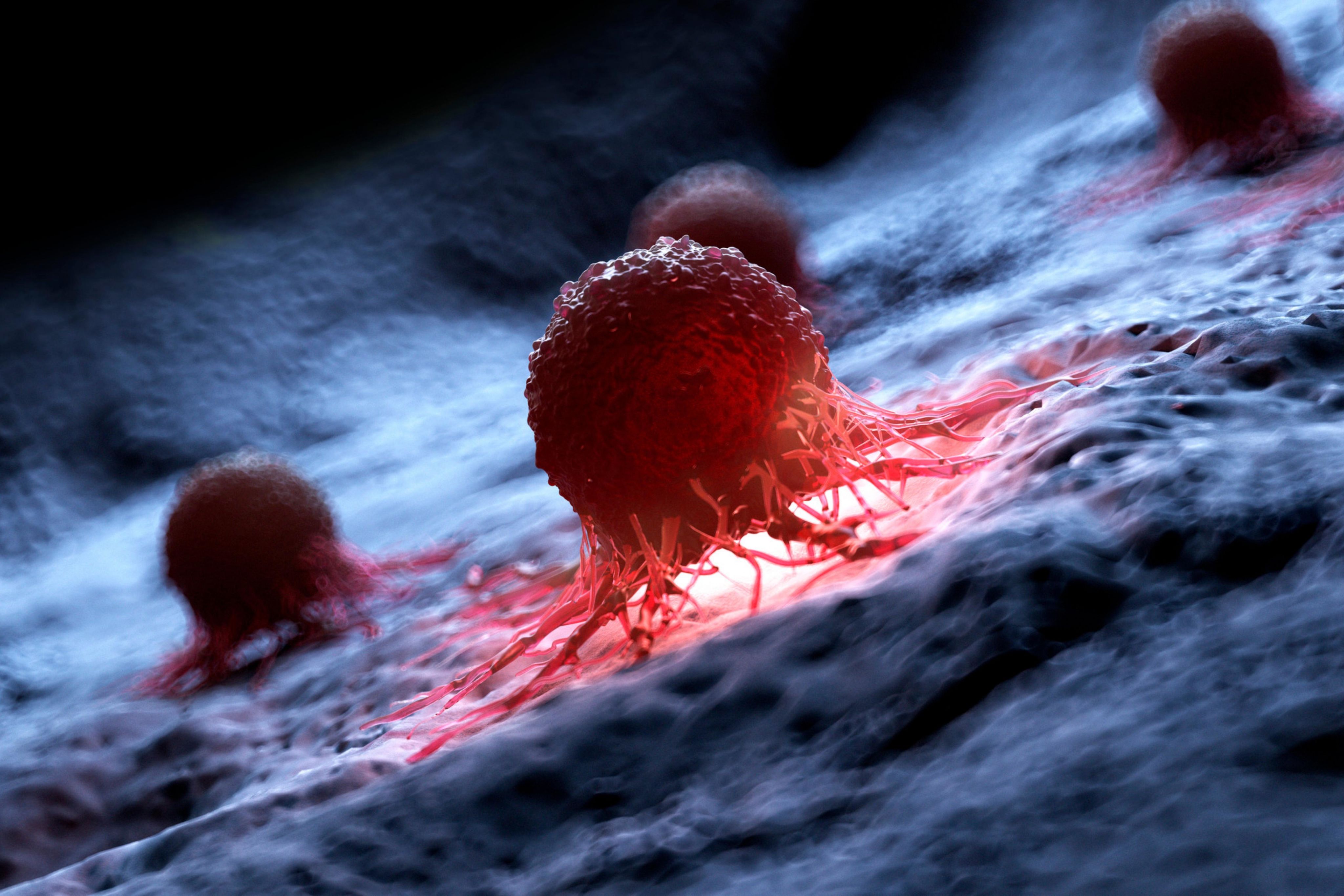
First, it destroys cancer cells.
Second, it weakens cancer cells with stem cell characteristics (so-called CSCs), which are responsible for disease recurrence and resistance to treatment.
Third, it activates the immune system.
Experiments have shown that after nsCaEP, the expression of heat shock proteins—HSP27 and HSP70—increases dramatically. These proteins, in addition to their protective function, act as alarm signals, attracting immune cells to the site of damage. In addition, the increased presence of the DEDD protein, which activates cell death pathways, including apoptosis, was observed.
This suggests that nsCaEP not only kills cancer mechanically but can also trigger a natural immune response - something like a "cancer vaccine".
Cancer stem cells - a formidable opponent
The biggest challenge of modern oncology is not so much cancer cells as a subset of cancer stem cells. These cells are responsible for recurrence, metastasis, and resistance to treatment.
In a study by a team of researchers from the Wroclaw University of Medical Sciences, the level of the marker CD133 - a hallmark of CSCs - decreased markedly after using nsEP without calcium.
– Our study showed a marked reduction in CD133 marker levels after using nanosecond electroporation (nsEP) – mainly without calcium. We know that nsEP affects the cell membrane and intracellular membranes, such as the endoplasmic reticulum, which contains essential calcium reservoirs. Therefore, an exciting future research direction will be to see if the release of calcium from these intracellular stores using nanosecond pulses can precisely destabilize ionic homeostasis in a subpopulation of cancer stem cells – says Dr. Anna Szewczyk.
Calcium added externally maintained CD133 expression. This paradox surprised scientists. It seems that calcium acts as a double agent—on the one hand, it disrupts the cell's homeostasis, and on the other hand, it protects its "stem identity."
– We plan to continue our research in this direction, analyzing not only the expression of CD133 but also the behavior of other tumor cell markers, their ability to renew and form colonies after treatment with both CaEP and nsEP – announces the researcher.
Why does calcium protect the "cancer core"? It is suspected to be a result of its interaction with mitochondria. CD133+ cells have a specialized protection system against oxidative stress and can use calcium to sustain their function. This is fascinating and disturbing, but it also provides new clues for research into a more precise attack on CSCs.

Two worlds collide: electricity and biology
What is most fascinating about this story is that the therapy's effectiveness is not based on expensive drugs but on simple measures: calcium salts and short electrical pulses. The whole thing could be called an "electric strike against cancer"—after all, the technique involves controlling the pulse's parameters: length, frequency, and voltage.
A nanosecond pulse changes a cell's biology faster than it has time to react. It's like sending a micro command to reset an ailing system.
From the lab to the hospital
In vitro results are an auspicious starting point, but, as the researchers point out, they have inherent limitations. The tumor microenvironment, the influence of the immune system, and the intercellular interactions present in a living organism can significantly alter the response to therapy.
– A well-known and widely accepted regimen after positive in vitro results is to move on to in vivo studies on an animal model and, in the longer term, develop pilot clinical trials with patients – explains Dr. Anna Szewczyk.
The Wroclaw team is actively working toward translating calcium electroporation research (CaEP) into clinical practice. To this end, the researchers are collaborating with, among others, veterinarians from Wroclaw University of Life Sciences, testing the safety and effectiveness of CaEP in animals. Already in 2019, thanks to the joint efforts of the Department of Molecular and Cellular Biology, led by Prof. Julita Kulbacka, and the team of Prof. Wojciech Kielan of the Wroclaw University Clinical Hospital, CaEP has been successfully applied according to the ESOPE standard (European Standard Operating Procedures of Electrochemotherapy) in the treatment of patients with pancreatic cancer.
A project funded by the Medical Research Agency made this possible. Importantly, this study has been officially registered in the international ClinicalTrials.gov database, paving the way for this therapy's further, more advanced evaluation stages.
– The results are auspicious, says Dr. Szewczyk, but further studies on an expanded group of patients are needed to confirm the efficacy and safety of this method in a clinical setting.
Is this the breakthrough we've been waiting for?
Although the research was conducted on cell lines in the laboratory, the results are extremely promising. Combining electrical pulses with calcium ions could become a cheap, selective, and effective method of fighting cancer - including those that resist classical therapy.
However, numerous questions stand in the way. How can the ideal pulse parameters be determined for a given type of cancer? Will the reaction observed in the laboratory be repeated in the human body? How can side effects be avoided? And above all, how can the therapy tame the effects on cancer stem cells?
One thing is sure: tumors do not like to be surprised. And a nanosecond pulse with added calcium is a very unpleasant surprise for them—not pills, not chemo, not a scalpel, just calcium, and an electrical pulse.
D. Sikora


FAQ: Calcium Electroporation in Cancer Treatment
What is calcium electroporation (CaEP), and how does it work in cancer treatment?
Calcium electroporation (CaEP) is a cancer treatment method that combines electrical impulses (electroporation) with the delivery of calcium ions to cancer cells. Electroporation temporarily permeabilizes the cell membrane by creating pores, allowing a rapid influx of extracellular calcium ions into the cells. This sudden increase in intracellular calcium disrupts normal calcium homeostasis, overloading mitochondria and depleting ATP (adenosine triphosphate), ultimately triggering various cell death pathways in cancer cells.
How does CaEP affect cancer cells' reactive oxygen species (ROS) levels and energy metabolism?
The study showed that nanosecond electroporation (nsEP), both with and without calcium, significantly increased the level of reactive oxygen species (ROS) in cancer cells (about a 5-fold increase). This increase in ROS correlated with a decrease in ATP production and indicated mitochondrial dysfunction. Microsecond CaEP (µsCaEP) and nsEP (with or without calcium) caused a significant reduction in ATP levels in cancer cell lines, suggesting that disruption of energy production is a key mechanism of CaEP's cytotoxic effects.
How does CaEP affect the expression of heat shock proteins (HSPs) in cancer cells?
Calcium electroporation, especially when combined with nanosecond pulses (nsCaEP), has increased the expression of heat shock proteins HSP27 and HSP70 in colon cancer cell lines. HSPs are typically produced in response to cellular stress and may play a role in cell protection and immune response activation. The overexpression of HSPs after CaEP suggests that the treatment induces stress in cancer cells and could stimulate an anti-tumor immune response by acting as damage-associated molecular patterns (DAMPs) after extracellular release.
How does CaEP affect the expression and localization of DNA binding protein containing death effector domain (DEDD)?
The study showed that the expression of DNA binding protein containing death effector domain (DEDD), which is associated with apoptosis, was significantly elevated in CaEP-treated cancer cells, especially after nanosecond CaEP (nsCaEP). Moreover, the localization of DEDD differed depending on the type of electroporation. After µsEP, DEDD was mainly cytoplasmic, while after nsCaEP, it was primarily located in the nucleus. This nuclear translocation of DEDD correlated with decreased cellular bioactivity, suggesting its role in mediating cell death pathways activated by nsCaEP.
What are the differences between microsecond (µsEP) and nanosecond (nsEP) electroporation in the context of CaEP?
The main difference lies in the level of cell penetration. Microsecond electroporation (µsEP) mainly affects the outer cell membrane, facilitating calcium entry from the extracellular environment. On the other hand, Nanosecond electroporation (nsEP) can also permeabilize intracellular organelles, including the endoplasmic reticulum (ER). Thus, nsEP can disrupt calcium stores in the ER and trigger calcium-induced calcium release, leading to a more pronounced increase in cytosolic calcium levels and potentially more efficient cell death. The study showed that nsEP is generally more effective than µsEP in reducing cancer cell viability and inducing oxidative stress.
What role does aspartate-β-hydroxylase (ASPH) play in CaEP-treated cancer cells?
Aspartate-β-hydroxylase (ASPH) is a calcium homeostasis protein often overexpressed in cancer cells. The study showed that CaEP, in particular nsEP, caused a significant increase in ASPH expression in drug-resistant colon cancer cells (LoVo Dx). In addition, ASPH was found to be strongly associated with mitochondria in both sensitive (LoVo) and drug-resistant cancer cells after CaEP treatment, suggesting that ASPH upregulation is associated with mitochondrial dysfunction induced by nsEP or CaEP.
What is the effect of CaEP on cancer stem cells (CSCs), as indicated by the CD133 marker?
Nanosecond electroporation (nsEP) without the addition of calcium dramatically reduced the expression of CD133, a marker of cancer stem cells (CSCs). This suggests that nsEP may be effective against this subpopulation of cells known for drug resistance and tumor recurrence. Interestingly, the addition of calcium during nsEP seemed to preserve CD133 expression, indicating a complex interaction between calcium influx and CSC markers that requires further study to understand the implications of targeting CSCs.
Is CaEP a promising option compared to existing treatment strategies for colorectal cancer?
The results of this study suggest that nanosecond calcium electroporation (nsCaEP) holds promise as an innovative treatment strategy for colorectal cancer, including drug-resistant forms. It has shown superior efficacy compared to microsecond CaEP in disrupting tumor cell viability, increasing oxidative stress, and inducing potential immune responses. Moreover, the ability of nsEP to reduce the CSC marker CD133 suggests the potential to target a stem cell population critical for tumor recurrence. Although further studies are needed to elucidate the underlying mechanisms and optimize protocols fully, nsCaEP's efficient

This material is based on an article:
Calcium electroporation induces stress response through upregulation of HSP27, HSP70, aspartate β-hydroxylase, and CD133 in human colon cancer cells
Anna Szewczyk, Nina Rembiałkowska, Jolanta Saczko, Małgorzata Daczewska, Vitalij Novickij, Julita Kulbacka
Biological Research
DOI: 10.1186/s40659-025-00591-9
Web. A. Hasiak
Photos: Tomasz Modrzejewski
www.freepik.com