Guardian of fluid balance
Lymph flow in heart failure
When we talk about circulation in the human body, we almost always mean blood. A complex network of arteries, veins, and capillaries that delivers oxygen and nutrients to every cell. But alongside this system, there is another, lesser-known but equally important system: the lymphatic system. It is responsible for removing excess fluid from tissues and maintaining the balance between what is in the blood vessels and what remains in the spaces between cells.
Only now are we beginning to understand how much this system can determine the course of one of the most dangerous diseases of our time: heart failure. The European Journal of Heart Failure published an article by researchers from the Wroclaw Medical University and Duke University School of Medicine entitled “Lower extremity lymphatic flow is associated with diuretic response in acute heart failure.” The authors show that the rate of lymph flow in patients' legs may correlate with their response to treatment. A relationship was found between lymph flow and whether diuretics (the primary tool in the treatment of acute heart failure) were effective or not.
When the heart loses its rhythm
In simple terms, heart failure is a condition in which the heart is unable to pump enough blood to meet the body's needs. One of the most troublesome and dangerous symptoms is fluid retention. Swelling of the legs occurs, and sometimes fluid accumulates in the abdomen or lungs, making breathing difficult.
The basic strategy of doctors is then to decongest the patient, i.e., to remove excess fluid. Diuretics, commonly known as water pills, are used for this purpose. The problem is that in some patients, these drugs work poorly or not at all. Despite high doses, urine is not excreted. This is called diuretic resistance.
Why does this happen? Until now, it was thought that the kidneys were mainly to blame, as they do not respond to the signals from the drugs. However, recent studies indicate that the lymphatic system, a delicate network of vessels running parallel to the veins, which is responsible for “collecting and transporting” excess fluid from the tissues and returning it to the bloodstream, may play an important role.
Podcast: Guardian of fluid balance
Lymph under fluorescent light
To examine how lymph behaves in patients with acute heart failure, a team from the Medical University of Wrocław and Duke School of Medicine used a modern diagnostic method: indocyanine green (ICG) lymphography. This method uses ICG, a fluorescent dye which, after being injected under the skin, travels with the lymph through the vessels. When illuminated with a special light, it glows like neon, allowing researchers to observe in real time how fast and how far the fluid travels.
The study included 65 patients hospitalized for acute heart failure. All received a standard dose of a diuretic (furosemide). Three hours later, they underwent lymphography of the legs. Then, for several hours, the amount of urine excreted and the decrease in body weight were measured.
The patients were divided into two groups: responders, i.e., those in whom the drugs worked properly, and non-responders, in whom the diuretics did not produce the expected effect. The differences in lymph flow between these groups proved to be very large. In almost all responders (95%), the lymph exceeded the ankle level within 10 minutes of dye administration, whereas in the non-responder group, this occurred in only 73%. This is even more evident when assessing significant flow, defined as the dye reaching at least 10 cm up the leg: it was found in 88% of patients who responded well to treatment, but only in 45% of the resistant group. The average distance traveled by lymph in 10 minutes was 50 cm in responders and only 10 cm in non-responders.
The conclusion is obvious: faster and more efficient lymph flow corresponded to greater diuretic efficacy.
“Our research indicates a significant link between faster lymph flow in the lower limbs and a better response to diuretic treatment in acute heart failure,” emphasizes Dr. Barbara Ponikowska, lead author of the study. “However, these results are preliminary, and it is still unclear whether efficient lymphatic drainage determines the effectiveness of diuretics or whether effective diuresis itself improves lymph flow.”
The lymphatic system as a “support pump”
This is a fundamental mechanism. To put it simply: diuretics remove water from the blood. When its volume decreases, the body must replenish the plasma for the process to continue. Where does this fluid come from? From the intercellular spaces, where it accumulates during edema. To remove it from there, efficient lymphatic transport is necessary.
If the lymphatic system is working well, the excess fluid returns to the blood, and the kidneys have something to filter. However, if the lymph flows slowly, the diuretic quickly depletes the plasma reserves, and the kidneys “turn off the tap” to prevent dehydration and collapse. It is this potential mechanism of resistance to diuretics that researchers from Wrocław have documented.
This can be compared to draining a flooded basement. The pump (diuretic) is working at full capacity, but if the drain pipe (lymphatic system) is clogged, the water has nowhere to flow to the pump, and the process comes to a standstill.
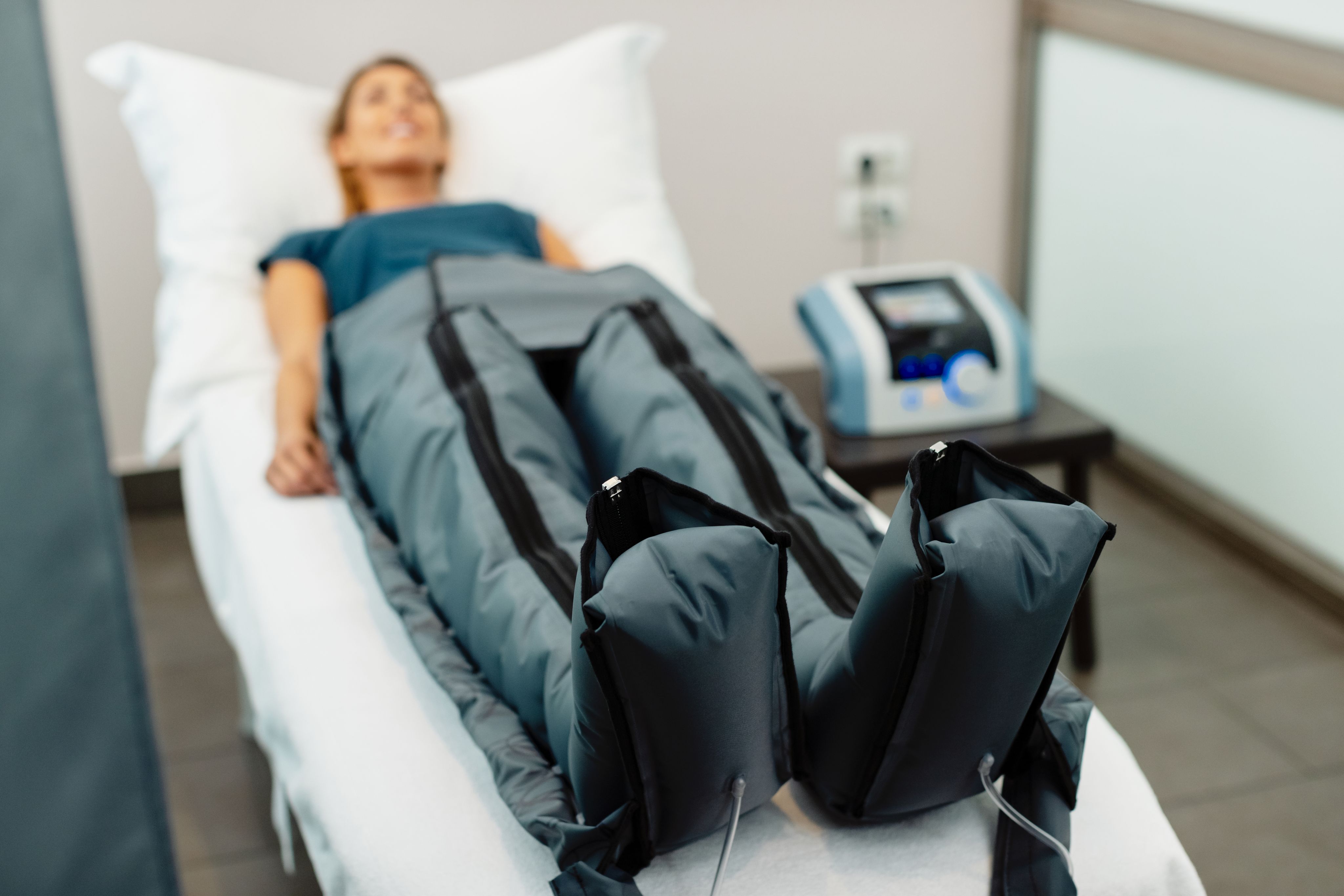
“Various therapeutic approaches aimed at improving lymphatic system function in heart failure are currently being tested,” says Dr. Ponikowska. “These include both physiotherapeutic methods, such as compression therapy and manual lymphatic drainage, as well as technological solutions, such as the eLym™ system. Pharmacotherapy research is focusing on VEGF-C/D agonists and drugs that improve lymphatic vessel contractility, among other things. However, this is only the beginning of the journey.
A hormone that inhibits lymph flow
The research team noticed another interesting correlation. Patients with poorer lymph flow had higher levels of aldosterone, a hormone produced in the adrenal glands that retains salt and water in the body. It is often responsible for the persistence of edema. High levels of this hormone are activated by the renin-angiotensin-aldosterone system (RAA), a defense mechanism of the body that often gets out of control in heart failure. Instead of protecting circulation, it promotes further fluid retention, increases blood pressure, and puts more strain on the heart. This creates a vicious cycle: the more aldosterone, the greater the edema and the more difficult the work of the lymphatic system.
“It can be assumed that modulation of the RAA system, including the use of aldosterone antagonists, may indirectly promote more effective lymphatic drainage,” notes Dr. Ponikowska. “However, there is currently no clinical data to confirm this hypothesis clearly.”
New therapeutic target
The study has its limitations. It was conducted in a single center on a relatively small group of patients, which makes it challenging to draw far-reaching conclusions and generalize them to the entire patient population. Therefore, it cannot yet be said that improvement in the functioning of the lymphatic system will automatically translate into better treatment, nor can a precise cause-and-effect mechanism be identified. It is also worth remembering that the method used – lymphography with indocyanine green – has its technical limitations, including the shallow penetration depth of the image. This may affect the results in people with more severe edema or obesity. Another challenge is the inability to perform repeated tests within a short period, which makes it difficult to monitor changes in lymph flow dynamics during therapy. Nevertheless, the research direction seems promising and opens up new avenues for understanding the pathophysiology of acute heart failure.
“We are currently conducting further research on the relationship between the lymphatic system and heart failure,” adds Dr. Ponikowska. “The key challenge is the lack of clinically available, non-invasive methods that would allow for continuous measurement of lymph flow. The development of such technologies could revolutionize the care of patients with AHF.”
An essential part of the circulatory system
For years, lymph has been mainly discussed in the context of oncology or lymphatic edema following surgery. This may determine the success of one of the key elements in treating a disease that affects millions of people worldwide.
It may be time to stop treating the lymphatic system as a secondary pathway of circulation and recognize it for what it really is: an essential element without which the fight against heart failure will not be complete. If further studies confirm these observations, the lymphatic system may become a new therapeutic target, not only supporting the work of the heart and kidneys, but even determining whether a patient will have a chance for effective decongestion. This represents a shift in perspective, from viewing the lymphatic system as an auxiliary system to recognizing it as an equal partner in maintaining circulatory health.
D. Sikora
M. D. Barbara Ponikowska, Department of Physiology and Pathophysiology, Wroclaw Medical University
M. D. Barbara Ponikowska, Department of Physiology and Pathophysiology, Wroclaw Medical University
Dr. Jan Biegus, MD, PhD, Institute of Heart Diseases, Wroclaw Medical University
Dr. Jan Biegus, MD, PhD, Institute of Heart Diseases, Wroclaw Medical University
FAQ: Guardian of fluid balance
What was the main objective of the study on lymphatic flow in acute heart failure (AHF)?
The main objective of the researchers was to test the hypothesis that in patients with acute heart failure (AHF), the effectiveness of diuretic treatment is related to lymphatic flow in the peripheral limbs. The study aimed to characterize lymph flow in the lower extremities and investigate the relationship between lymph flow characteristics and early unloading potential.
How were patients classified as responders or non-responders to diuretics in the study?
Patients were classified based on diuretic efficacy, which was defined as cumulative diuresis and weight loss. Patients with cumulative diuresis ≥900 ml within 6 hours after furosemide administration were classified as responders to diuretics. Those with diuresis between 600 and 900 ml were also included in this group if their weight loss exceeded 1 kg within 24 hours. The remaining patients who did not meet these criteria were classified as non-responders to diuretics.
What is the main conclusion from the study on the relationship between lymphatic flow and response to diuretics in acute heart failure?
For the first time, it has been shown that faster and more extensive lymph flow in the lower limbs was associated with better diuretic efficacy in acute heart failure (AHF). The researchers suggest that the lymphatic system may play a crucial role in the process of decongestion and could become a potential therapeutic target to enhance decongestion in patients with AHF.
What factors were independently associated with lymph flow distance and response to diuretics?
Multivariate analyses found that serum aldosterone levels (negatively) and tricuspid annular plane systolic excursion (TAPSE) (positively) were independently associated with lymph flow distance in the lower extremities. Furthermore, lymph flow distance over 10 minutes (per 10 cm of change) and aldosterone levels (negatively) were independent predictors of belonging to the diuretic-responsive group.
How was lymphatic flow in the lower limbs assessed in the study patients?
Lymphatic flow in the lower limbs was assessed using indocyanine green (ICG) lymphography, a validated method for visualizing lymphatic drainage. Indocyanine green (ICG) dye was injected subcutaneously into three specific sites on the foot, and ICG propagation in the lymphatic vessels was monitored for 10 minutes using the IC-Flow™ imaging system. Lymph flow was defined as “present” when it reached the ankle and “significant” when it traveled more than 10 cm within 10 minutes of dye injection. Lymphography was performed 3 hours after bolus administration of the diuretic.
What key differences were observed in lymph flow between diuretic responders and non-responders?
There were significantly more patients with present or significant lymph flow in the diuretic-responsive group (95% vs. 73% and 88% vs. 45% in the non-responsive group, respectively; p < 0.01). Responders also had a significantly longer median distance traveled by lymph in 10 minutes (50 cm [24–75] vs. 10 cm [3–38]; p < 0.0005). The percentage of patients whose lymph reached each of the predefined lower limb levels was significantly higher in the diuretic-responsive group (e.g., to the knee 70% vs. 27%; all p < 0.05).
What role does the lymphatic system play in fluid homeostasis and heart failure?
The lymphatic system plays a key role in fluid homeostasis by maintaining fluid balance between the interstitial and intravascular spaces. In a healthy state, it collects and removes transudate from the interstitial space in peripheral tissues, transporting it to the central venous system. Dysfunction of the lymphatic system can lead to fluid accumulation in the interstitial tissues, which clinically manifests as peripheral edema (congestion), a significant feature of heart failure.
Materiał powstał na podstawie artykułu:
Lower extremity lymphatic flow is associated with diuretic response in acute heart failure
Barbara Ponikowska, Robert Zymliński, Marat Fudim, Beata Ponikowska, Gracjan Iwanek, Mateusz Guzik, Jan Biegus
European Journal of Heart Failure
DOI: doi.org/10.1002/ejhf.3655
PoweredNotebook LM.
Web. A. Maj
Photos: Freepik